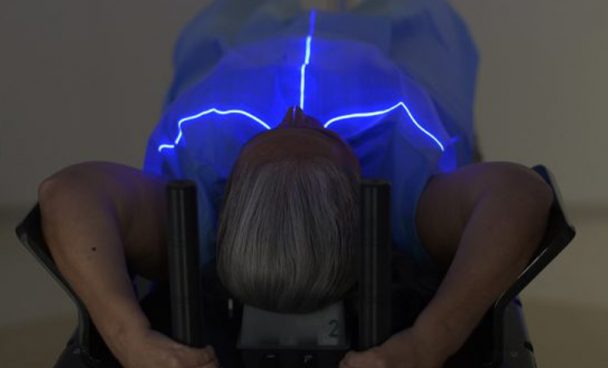
How Radiotherapy is Done
Radiotherapy is a treatment that uses ionizing radiation (a type of energy) to destroy or disable the duplication of tumor cells, to control pain caused by some types of cancer, and also to reduce the size of tumors that are compressing an organ. In it, the DNA of cancer cells is targeted by the radiation, which prevents their reproduction – as a result, they stop developing.
Some healthy cells may also be affected during radiotherapy, but to a lesser extent. Although they have a greater capacity for recovery, in some treatments the sessions are fractionated to give the body time to recover.
Additionally, the radiation doses and the application time are calculated according to the type and size of the tumor, which also helps preserve healthy cells.
According to the WHO (World Health Organization), approximately 60% of patients diagnosed with cancer will undergo radiotherapy at some stage of their treatment. It is worth noting that this procedure is painless.
Benefits of Radiotherapy
The results of radiotherapy are often very positive: the tumor can disappear, and the disease can be controlled or even cured, as is done in breast radiotherapy or prostate radiotherapy, etc.
When a cure is not possible, radiotherapy can contribute to a better quality of life, as its applications reduce the size of the tumor, which relieves pressure, reduces bleeding, pain, and other symptoms of certain types of cancer, providing relief to patients.
The situations in which radiotherapy is most commonly used are:
- Exclusive – when it is used as the sole treatment for cancer;
- Curative or radical – when radiotherapy is considered the main tool in combating cancer;
- Neoadjuvant – when it is performed before surgery, to reduce the size of the tumor (may or may not be combined with chemotherapy);
- Adjuvant – when it is performed after surgery (with or without the combination of chemotherapy), to reduce the risk of recurrence by interrupting the growth of any remaining cancer cells;
- In combination with other treatments – such as chemotherapy (chemoradiotherapy), without surgery involvement; and
- Palliative use – in patients with advanced cancer, as a way to relieve symptoms.
Types of radiotherapy
There are several types of radiotherapy. Understand them below.
External beam radiotherapy consists of emitting a beam of radiation externally and at a long distance, usually of X-rays or high-energy electrons, produced by a machine called a linear accelerator. The target is the tumor. Most people undergoing radiotherapy receive this type of treatment.
The patient lies on a treatment table and the radiation is emitted by the linear accelerator, positioned at a safe distance from the person. Applications are usually daily, but the number of sessions and intervals are determined on a case-by-case basis.
Technology in Radiation Therapy Precision
To plan the treatment, the tumor and adjacent healthy organs are identified using computed tomography (CT). With this information, dedicated software calculates the precise distribution of radiation in the patient. Reference points are marked on the skin to assist in positioning the linear accelerator.
A plastic mask mold may be made to ensure that radiation reaches only the area to be treated, sparing the surrounding healthy tissue, especially when targeting the head and neck region. In this case, the area to be treated is marked directly on the mask, not on the skin. In other areas of the body, localization accessories such as vacuum mattresses and fixation supports may be necessary.
External beam radiotherapy is another modality of radiotherapy and has several subtypes, which are:
- Conventional radiotherapy (2D-RT) – of lower complexity, it uses simple radiographic images or even topographic anatomy to identify the target. It usually involves large radiation fields and greater involvement of healthy tissues;
- Conformal or three-dimensional radiotherapy (3D-CRT) – uses computed tomography for treatment planning, which consists of static incidences of radiation beams that, combined, encompass the target area;
- Intensity-modulated radiation therapy (IMRT) – a type of treatment where the treatment dose can be modulated for heterogeneous targets, allowing for reduced incidence in healthy tissues near tumors and dose escalation;
- Volumetric arc therapy (VMAT) – an IMRT technique in which radiation is delivered in a dynamic arc, with the linear accelerator’s gantry moving during the session. It typically has a faster dose delivery in treatment;
- Radiosurgery – a technique for the high-precision treatment of cranial lesions, such as metastases, benign tumors, and arteriovenous malformations, without the need to open the skull. It usually lasts from one to five sessions;
- Extracranial stereotactic radiotherapy – a technique that also requires high precision, performed in few fractions, for radical or palliative ablative (tumor destruction) treatment of primary or metastatic tumors. Used in lung tumors, liver, lymph nodes, and in metastases in general;
- Image-guided radiotherapy (IGRT) – a technique that incorporates imaging at the time of dose delivery, ensuring better precision and reducing the need for more generous safety margins. Digital radiographs, ultrasound, or cone beam tomographies can be used, incorporated into the linear accelerator; and
- Total Body Irradiation (TBI) – a technique used in preparation for bone marrow transplantation to reduce the risk of rejection.
Another type of radiotherapy is internal radiotherapy or brachytherapy, which uses internal radiation sources placed very close to or in direct contact with the target – unlike external radiotherapy, where the radiation source is far from the target. It also requires simulation to choose the best approach.
In brachytherapy, the radioactive material used is in the form of seeds, wires, or plates and is delivered through catheters, applicators, or needles. It is often indicated for the treatment of prostate cancer, retinoblastoma, gynecological tumors, head and neck cancer, sarcomas, choroidal melanoma (inside the eyes), skin cancer, and sarcomas, among others.
It is usually said that in brachytherapy, the radiation goes from the inside out and in external beam radiation therapy, from the outside in.
Finally, intraoperative radiotherapy is the technique in which radiotherapy is administered during the surgical procedure. It can use electron beam therapy, brachytherapy, or orthovoltage equipment.
Difference between chemotherapy
Both treatments aim to reduce the reproductive capacity of cancer cells, but they are quite different. Chemotherapy uses drugs that reach all cells in the body through the bloodstream. In contrast, radiotherapy uses ionizing radiation, which affects only the areas where it is applied. Radiotherapy is generally more indicated for controlling local or regional disease.
Possible Adverse Effects and Complications
Radiation therapy can have adverse effects, which depend on the part of the body exposed to it and the amount of radiation used. Most of these effects are temporary, can be controlled, and usually disappear after the end of treatment.
Here are some of the most commonly observed adverse effects in oncology patients undergoing radiation therapy:
- Any area – hair loss and loss of hair at the treatment site (sometimes permanent), skin irritation at the application site, and fatigue;
- Head and neck – dry mouth, thickening of saliva, difficulty swallowing, sore throat, changes in taste, nausea, mouth sores, tooth decay;
- Chest – difficulty swallowing, cough, shortness of breath;
- Stomach and abdomen – nausea, vomiting, diarrhea;
- Pelvis – diarrhea, bladder irritation, frequent urination, sexual dysfunction, rectal irritation; and
- Breast – fatigue, skin changes, edema, and sensitivity.